Barrett’s Esophagus
Barrett’s Esophagus Cancer Risk: Understanding Dysplasia and Your Next Steps
Understanding Barrett’s esophagus cancer risk starts with dysplasia—and how personalized risk assessment may guide your care.
Barrett’s esophagus is a condition in which the lining of the esophagus changes, often as a result of long-term acid reflux (GERD). Over time, repeated exposure to stomach acid can cause the normal esophageal lining to be replaced with tissue that more closely resembles the lining of the intestine.
Barrett’s esophagus itself does not cause cancer but it is considered a precancerous condition, meaning it can increase the risk of developing esophageal cancer in some individuals.
Most people with Barrett’s esophagus will never develop cancer. However, understanding your personal cancer risk—and how that risk is monitored—is an important part of managing the condition.
One of the most important ways doctors assess Barrett’s esophagus cancer risk is by identifying changes called dysplasia.
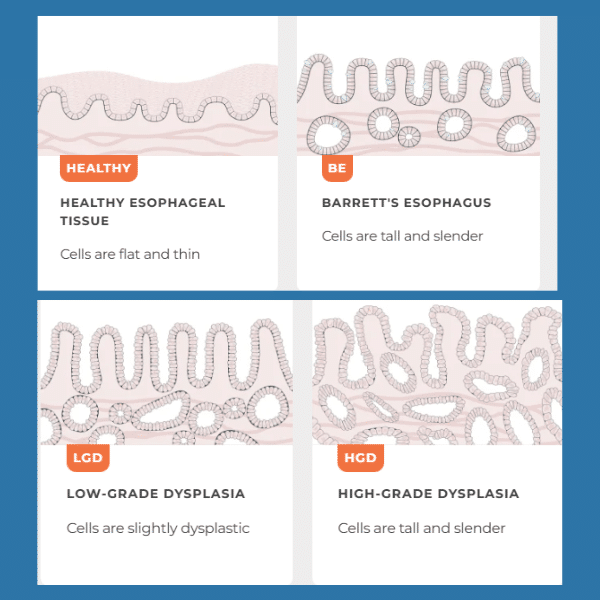
What Is Dysplasia in Barrett’s Esophagus?
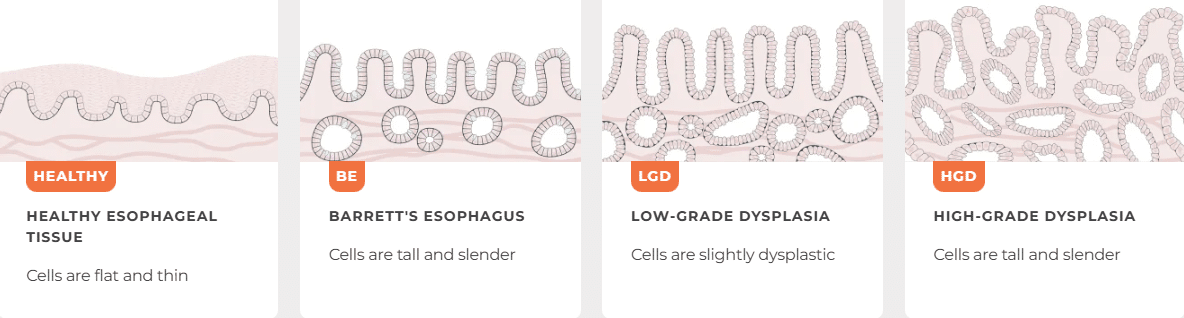
How Barrett’s esophagus can progress from normal tissue to low-grade and high-grade dysplasia, with increasing risk of esophageal cancer.
Factors that influence Barrett’s esophagus cancer risk include:
- Age
- Weight
- Sex
- Presence of a hiatal hernia
- Family history
- Length of the Barrett’s segment
These factors help guide care but they don’t always reflect an individual’s true risk.
Personalized Cancer Risk: Looking Beyond Dysplasia
TissueCypher is an advanced test that evaluates molecular changes in Barrett’s esophagus tissue to help predict a patient’s individual risk of progression.
Unlike traditional biopsy grading, which looks at how cells appear under a microscope, TissueCypher can detect changes that may occur before dysplasia becomes visible.
The test provides:
- A risk score (1–10)
- A risk category: low, intermediate, or high
- A 5-year probability of progression to: High-grade dysplasia (HGD); Esophageal adenocarcinoma (EAC)
Why this matters:
Low-risk patients may be able to extend surveillance intervals
High-risk patients may benefit from earlier treatment—even without dysplasia
Are You at Risk for Barrett’s Esophagus?
This discussion guide can be used to assist you in a
conversation with your healthcare professional to determine
if TissueCypher Barrett’s esophagus test is right for you.
Shared-Decision Making Made Easy: Jump Start the Conversation with Your Healthcare Provider.
Are You at Risk for Barrett’s Esophagus?
Barrett’s esophagus (BE) develops from chronic acid reflux (GERD), even in people who don’t experience typical heartburn.
The American Gastroenterological Association recommends considering endoscopic screening (EGD) if you have three or more risk factors, including:
- Long-standing acid reflux
- Age over 50
- Male sex
- White race
- Abdominal obesity
- Smoking history
- Family history of Barrett’s esophagus or esophageal cancer
Already Diagnosed with Barrett’s Esophagus?
- Barrett’s esophagus is not cancer, but it is a precancerous condition.
- Only about 1 in 40 patients progress to cancer over 5 years. However, if cancer develops, outcomes can be serious.
- The key: understanding your personal risk and managing it early
Not All Barrett’s Esophagus Is the Same
Your pathology results may include:
- Non-dysplastic Barrett’s esophagus
- Indefinite for dysplasia
- Low-grade dysplasia
Each category carries a different level of risk, which is why personalized assessment matters.
The TissueCypher Barrett’s Esophagus Test is one tool clinicians use to better understand your individual risk of progression and guide next steps.
Start a Shared Decision-Making Conversation
The most important step you can take is to have an informed conversation with your healthcare professional.
Download the Barrett’s Esophagus Discussion Guide
Use this guide to:
- Understand your diagnosis and risk level
- Ask the right questions about monitoring and treatment
- Explore whether additional risk assessment tools are appropriate
- Make confident, informed decisions together with your care team
Bring This Guide to Your Appointment
Print or save the discussion guide and review it with your doctor.
Better conversations lead to better care.
Surveillance: Monitoring Barrett’s Esophagus
All patients with Barrett’s esophagus typically undergo regular upper endoscopy with biopsies.
This helps:
- Detect progression early
- Identify dysplasia
- Guide treatment decisions
- Patients at higher risk are monitored more frequently.
Treatment for Barrett’s Esophagus: Endoscopic Eradication Therapy (EET)
Endoscopic eradication therapy (EET) is a minimally invasive and highly effective treatment for Barrett’s esophagus.
EET typically includes:
Endoscopic mucosal resection (EMR)
Removal of abnormal or suspicious tissue during endoscopy
Ablation therapy
Destruction of remaining Barrett’s tissue so healthy tissue can regrow
Benefits of EET:
Helps prevent progression to esophageal cancer
Reduces the need for invasive surgery (esophagectomy)
Provides durable, long-term results
Key Takeaways on Barrett’s Esophagus Cancer Risk
- Dysplasia is the primary way cancer risk is assessed
- High-grade dysplasia carries the highest risk
- Risk varies significantly between individuals
- Personalized tools like TissueCypher can refine risk
- Early detection and treatment can help prevent cancer
If you or a loved one are living with chronic acid reflux, GERD, or ongoing heartburn, it’s worth having a conversation with your healthcare provider about your risk and whether further evaluation makes sense.
Resources
The Hidden Risk of Chronic GERD/Heartburn
In part 2 of our 4-part series on GERD and Barrett’s Esophagus, we take a closer look at what Barrett’s esophagus is, how it develops from chronic acid reflux, and why early detection is essential to reducing the risk of esophageal cancer.
Barrett’s Esophagus Cancer Risk: Understanding Dysplasia and Your Next Steps
Most people with Barrett’s esophagus will never develop cancer. However, understanding your personal cancer risk—and how that risk is monitored—is an important part of managing the condition. One of the most important ways doctors assess Barrett’s esophagus cancer risk is by identifying changes called dysplasia.
Personalized Progression Risk Assessment
TissueCypher is an AI-driven precision medicine test that predicts the risk of progression to cancer in patients with Barrett’s esophagus. The test has the power to improve the standard of care for Barrett’s esophagus patients, many of whom are misclassified by traditional risk assessment.
Barrett's Esophagus on Medline Plus
Barrett esophagus (BE) is a disorder in which the lining of the esophagus is damaged by stomach acid leading to changes in the cells of the lining. The esophagus is also called the food pipe, and it connects your throat to your stomach.
Listen to our
latest Podcast!
This will close in 20 seconds