Hepatitis C: 8 Common Questions Answered
1. What is the difference between hepatitis A, B, and C?
The term “hepatitis” means inflammation of the liver. There are three commonly known viruses called hepatitis A, hepatitis B, and hepatitis C that cause the liver to become inflamed.
Hepatitis A causes acute (short-term) inflammation of the liver. It is very contagious and can spread from contaminated food or water, or from contact with someone who has the virus. Symptoms include fatigue, nausea, and abdominal pain. Hepatitis A usually resolves on its own after 1-2 months and a vaccine is available.
Hepatitis B can be acute and chronic (ongoing). It spreads through blood and other bodily fluids and can cause yellowing of the eyes, dark urine, and abdominal pain. It is preventable by a vaccine and often clears up on its own.
Hepatitis C is typically chronic and only spreads through blood. The treatment is rapidly evolving and includes antiviral medications. There is currently no vaccine.
2. What are the risk factors for hepatitis C?
Hepatitis C is spread by contact with contaminated blood. Intravenous (IV) drug use is the most common way that hepatitis C is transmitted. Other risk factors for hepatitis C include high-risk sexual behavior, jobs that require contact with blood (e.g. healthcare workers), and the sharing of razors or other personal items with someone who has hepatitis C.
3. What are symptoms of hepatitis C?
Most people with hepatitis C do not have any symptoms until the disease progresses. Those who do experience symptoms may have abdominal pain, fatigue, poor appetite, or jaundice (yellowing of the skin and whites of the eyes). Once a person with hepatitis C develops cirrhosis, they may also have muscle weakness, abdominal swelling, nausea, and weight loss.
4. How is hepatitis C diagnosed?
An initial blood test can detect the presence of hepatitis C. Then, additional blood tests will be used to measure the amount of virus in your blood (called the viral load) and to figure out the genetic variation of the virus (called genotyping).
5. How is hepatitis C treated?
According to the Centers for Disease Control and Prevention (CDC), “current treatments usually involve just 8–12 weeks of oral therapy (pills) and cure over 90% with few side effects.”
The research on hepatitis C treatment continues to evolve, so it’s best to talk to your doctor about the latest available treatment options.
6. Should those with hepatitis C be restricted from certain working environments?
The current recommendations state that those with hepatitis C do not need to be kept from work, school, or child care settings. There is currently no evidence that the virus can be transmitted by those who handle food or provide other services, unless there is blood to blood contact.
7. Can those with hepatitis C drink alcohol?
Alcohol can speed up liver damage in those with hepatitis C and should be avoided.
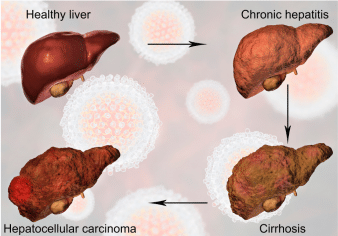
8. Does hepatitis C cause cirrhosis?
Hepatitis C can cause cirrhosis (scarring) of the liver in some people. Those who are co-infected with HIV or hepatitis B, drink alcohol, or are obese are at a higher risk of developing cirrhosis.
Your doctor will recommend a treatment plan for cirrhosis that may include medications, as well as diet and lifestyle modifications to help treat the symptoms and slow down the progression of the disease. In some cases of severe liver disease, a liver transplant may be considered.
If you have hepatitis C, it’s important to work with your healthcare team to develop a plan of action early on to help prevent severe liver damage and other potential health complications.
Related Resources
 Katelyn Collins, RD is a registered dietitian and health writer specializing in digestive health. Katelyn’s personal experience with a digestive condition first sparked her passion for nutrition and health. Since then, she has been a vocal advocate for the digestive health community and has dedicated her own nutrition practice to serving those with digestive conditions.
Katelyn Collins, RD is a registered dietitian and health writer specializing in digestive health. Katelyn’s personal experience with a digestive condition first sparked her passion for nutrition and health. Since then, she has been a vocal advocate for the digestive health community and has dedicated her own nutrition practice to serving those with digestive conditions.
Listen to our
latest Podcast!