I’m Talking about Poop
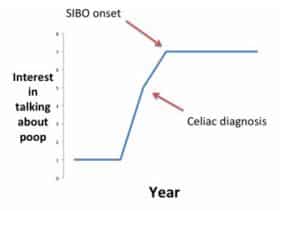
Since being diagnosed with celiac disease in 2009 and experiencing small intestinal bacterial overgrowth from 2010 – 2013, the amount of time I spent thinking and talking about my bowel functions skyrocketed. It could be compared to the meteoric rise in gluten-free products on store shelves in the last five years. If there were a graph displaying my comfort level with talking about poop over my lifetime, it would look like this:
What I found surprising after my diagnosis was that GI troubles – poop, gas, pain, hemorrhoids, rectal bleeding, colostomies – are more taboo than I ever realized. I would say that people are even more uncomfortable discussing their gastrointestinal symptoms than they are discussing their sex life. And until you experience chronic gastrointestinal distress, you may not feel any need to talk about poop. But once you do, there’s no turning back.
It’s amazing how healing it is to speak with others about what’s troubling you, have someone else express their concern for your troubles, and even more so if they relate to what you’re experiencing. Addicts feel freedom talking with other addicts. Cancer survivors find solace with those who have experienced the same trauma. Veterans routinely hang out at Veterans hospitals to feel a part of their community. Why shouldn’t there be a community for sharing about poop problems?
While not everyone can say they’ve survived a horrific accident, I do think that most people can relate to having to run to the bathroom on occasion, feeling grumpy from constipation, or being embarrassed by smelly gas. Probably fewer people can say they’ve had fecal incontinence – pooped their pants – or have been afraid to leave the house for fear of being far from a bathroom. This community knows the importance of keeping extra plastic bags, wet wipes and a change of underwear in the car glove compartment just for such emergency situations. They also know the isolation felt from others exclaiming “gross!”, “ew!”, or “not before we eat!”, as if there’s ever a good time to talk about it. Even more so, gastrointestinal troubles often happen more than once in a day and several days in a row. They can turn a good day to a bad day in a heartbeat. If you can relate with anything I’ve said here, please consider finding a support group or community of those with a similar condition. Speaking your truth can set you free. And if you haven’t told your doctor yet about these problems, please know that EVERY HEALTH PROVIDER TALKS ABOUT POOP. There is no one less embarrassing to speak with about your poop than your doctor, your nurse, or your dietitian.
Janelle Smith is a Registered Dietitian Nutritionist (RDN) based in Los Angeles, CA , specializing in gastrointestinal disorders, food allergies, eating disorders, intuitive eating, and other challenges to living with restricted diets. Her philosophy is an integrated approach of psychology, behavioral change, and diet to achieve a peaceful relationship with food, with the goal of a least-restrictive diet that improves both physical and mental health. This article first appeared on her blog.
Listen to our
latest Podcast!