Barrett’s Esophagus Cancer Risk: Understanding Dysplasia and Your Next Steps
Understanding Barrett’s esophagus cancer risk starts with dysplasia—and how personalized risk assessment may guide your care.
What Is Barrett’s Esophagus?
Barrett’s esophagus is a condition in which the lining of the esophagus changes, often as a result of long-term acid reflux (GERD). Over time, repeated exposure to stomach acid can cause the normal esophageal lining to be replaced with tissue that more closely resembles the lining of the intestine.
Barrett’s esophagus itself does not cause cancer but it is considered a precancerous condition, meaning it can increase the risk of developing esophageal cancer in some individuals.
Most people with Barrett’s esophagus will never develop cancer. However, understanding your personal cancer risk—and how that risk is monitored—is an important part of managing the condition.
One of the most important ways doctors assess Barrett’s esophagus cancer risk is by identifying changes called dysplasia.
What Is Dysplasia in Barrett’s Esophagus?
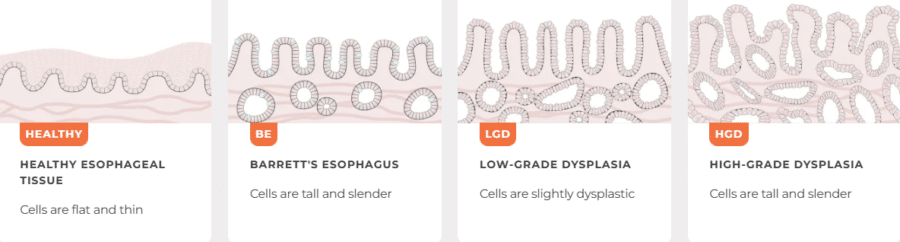
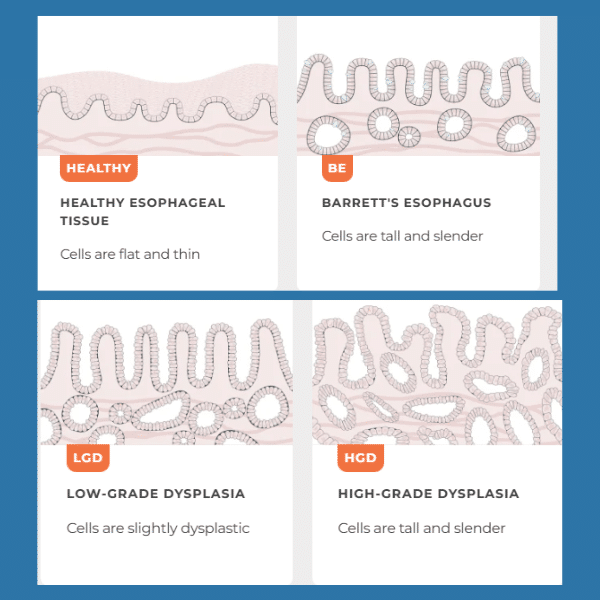
How Barrett’s esophagus can progress from normal tissue to low-grade and high-grade dysplasia, with increasing risk of esophageal cancer.
Dysplasia refers to abnormal changes in the cells lining the esophagus. In Barrett’s esophagus, dysplasia is used to estimate the risk of progression to esophageal cancer.
Dysplasia is typically classified into three categories:
- No dysplasia – Barrett’s cells are present, but no precancerous changes are seen
- Low-grade dysplasia (LGD) – Early precancerous changes are present
- High-grade dysplasia (HGD) – Advanced precancerous changes with the highest cancer risk
Factors that influence Barrett’s esophagus cancer risk include:
- Age
- Weight
- Sex
- Presence of a hiatal hernia
- Family history
- Length of the Barrett’s segment
These factors help guide care but they don’t always reflect an individual’s true risk.
Personalized Cancer Risk: Looking Beyond Dysplasia
TissueCypher is an advanced test that evaluates molecular changes in Barrett’s esophagus tissue to help predict a patient’s individual risk of progression.
Unlike traditional biopsy grading, which looks at how cells appear under a microscope, TissueCypher can detect changes that may occur before dysplasia becomes visible.
The test provides:
- A risk score (1–10)
- A risk category: low, intermediate, or high
- A 5-year probability of progression to: High-grade dysplasia (HGD); Esophageal adenocarcinoma (EAC)
Why this matters:
Low-risk patients may be able to extend surveillance intervals
High-risk patients may benefit from earlier treatment—even without dysplasia
Barrett’s Esophagus Monitoring vs Treatment
The decision to monitor or treat Barrett’s esophagus depends on an individual’s risk of progression to cancer.
This decision is typically based on:
- Dysplasia grade
- Clinical risk factors
- Endoscopy findings
- Personalized risk tools
Surveillance: Monitoring Barrett’s Esophagus
All patients with Barrett’s esophagus typically undergo regular upper endoscopy with biopsies.
This helps:
- Detect progression early
- Identify dysplasia
- Guide treatment decisions
Patients at higher risk are monitored more frequently.
Treatment for Barrett’s Esophagus: Endoscopic Eradication Therapy (EET)
Endoscopic eradication therapy (EET) is a minimally invasive and highly effective treatment for Barrett’s esophagus.
EET typically includes:
Endoscopic mucosal resection (EMR)
Removal of abnormal or suspicious tissue during endoscopy
Ablation therapy
Destruction of remaining Barrett’s tissue so healthy tissue can regrow
Benefits of EET:
- Helps prevent progression to esophageal cancer
- Reduces the need for invasive surgery (esophagectomy)
- Provides durable, long-term results
Key Takeaways on Barrett’s Esophagus Cancer Risk
- Dysplasia is the primary way cancer risk is assessed
- High-grade dysplasia carries the highest risk
- Risk varies significantly between individuals
- Personalized tools like TissueCypher can refine risk
- Early detection and treatment can help prevent cancer
If you or a loved one are living with chronic acid reflux, GERD, or ongoing heartburn, it’s worth having a conversation with your healthcare provider about your risk and whether further evaluation makes sense.
Related Resources:
Barrett’s Esophagus Health Hub
Barrett’s Esophagus: The Hidden Risk of Chronic GERD/Heartburn
Barrett’s Esophagus Risk Factors
Barrett’s Esophagus Treatment Options
Take Control of Barrett’s Esophagus
This education initiative was created with support from Castle BioSciences.
Featured Podcast Episodes
View Podcast episodes related to Barrett’s Esophagus.
April 1, 2026
GERD to Barrett’s Esophagus: A Patient Story That Could Change Your Care
Barrett’s esophagus can develop silently in people with chronic acid reflux (GERD)—and many don’t realize their risk until after diagnosis. In this episode of Gastro Girl, Robin shares her powerful, real-life journey from ongoing reflux symptoms to a diagnosis of Barrett’s esophagus—and how that moment changed everything. Like many patients, Robin faced confusion, fear, and unanswered questions about what her diagnosis meant and what to do next. After learning more about Barrett’s esophagus, including risk factors, monitoring, and emerging tools like TissueCypher, she felt empowered to take a more active role in her care and have informed conversations with her healthcare team. In this episode, you’ll learn: – What Barrett’s esophagus is and how it relates to GERD – Common symptoms and warning signs patients often overlook – What a diagnosis means for cancer risk and monitoring – How patient education can transform fear into action – Why self-advocacy matters in digestive health care Robin’s story is a reminder that knowledge can change your path—and your outcomes. If you experience chronic heartburn or reflux, this episode offers important insights to help guide your next conversation with your doctor. This educational series is supported by Castle Biosciences. Robin’s story reflects her personal experience. Gastro Girl provides evidence-based information to support informed patient-provider conversations and does not offer medical advice.
February 13, 2026
Barrett’s Esophagus in the U.S.: How GERD Increases Cancer Risk
Chronic heartburn and GERD are often brushed off as everyday issues—but for some patients, long-term reflux can quietly progress to Barrett’s esophagus, the only known precursor to esophageal cancer. In Part 1 of this 4-part U.S.-focused patient education series, foregut surgeon Dr. Dan Lister, Founder of the Arkansas Heartburn Treatment Center, explains how reflux disease can evolve over time and why early recognition matters. In this episode, you’ll learn: – How chronic GERD can progress silently – Why Barrett’s esophagus matters—even when symptoms improve or disappear – Key warning signs patients should never ignore – How Barrett’s is detected and risk is assessed in the U.S. – Treatment approaches that may help reduce cancer risk Whether you’ve lived with reflux for years or are newly diagnosed, this episode provides clear, evidence-based guidance to help you take reflux seriously—and take action. This episode is part of a 4-part patient education series sponsored by Castle Biosciences and produced in collaboration with leading U.S. clinicians dedicated to improving outcomes for patients with Barrett’s esophagus.
June 17, 2025
Barrett’s Esophagus: What Patients Need to Know to Take Action
In the final episode of our 4-part series on GERD and Barrett’s Esophagus, we move beyond awareness to focus on action. What should patients actually do after diagnosis—and how can they take charge of their care journey? We’re joined by Tedra Gray, a seasoned Advanced Practice Provider, who shares real-world examples and practical advice for patients navigating chronic reflux, Barrett’s Esophagus, or treatment follow-up. You’ll learn: – Why early diagnosis and follow-up matter – What can happen if Barrett’s Esophagus is left untreated – How shared decision-making helps build the right care plan – The different approaches for patients at low, moderate, or high risk Whether you’re newly diagnosed or managing long-term reflux, this episode offers compassionate, expert-backed guidance to help you feel informed and empowered. Missed the earlier episodes? Scroll to the bottom of this page to listen or watch now. This series is sponsored by Castle Biosciences and produced in collaboration with leading clinicians and researchers committed to improving patient outcomes.
June 10, 2025
Managing Barrett’s Esophagus: Treatments & Risk Reduction
In Part 3 of our 4-part series on GERD and Barrett’s Esophagus, we’re joined by Dr. Caitlin Houghton, a foregut surgeon with Keck Medicine of USC, to discuss what happens after Barrett’s Esophagus is diagnosed—and how patients can reduce their cancer risk and manage the condition effectively. From reflux control to endoscopic eradication therapy (EET), and in some cases, surgery, Dr. Houghton breaks down the latest treatment strategies and what patients need to know. This episode offers practical advice, expert insights, and real hope for those navigating life with Barrett’s. Topics include: – What Barrett’s Esophagus is and why it matters – How doctors decide when and how to treat – The role of EET, medications, and lifestyle changes – When surgery may be necessary – Tips for patients to advocate for their care Missed the earlier episodes? Scroll to the bottom of this page to listen or watch now. This series is sponsored by Castle Biosciences and produced in collaboration with leading clinicians and researchers committed to improving patient outcomes.
June 3, 2025
Barrett’s Esophagus: The Hidden Risk of Chronic Heartburn
In part 2 of our 4-part series on GERD and Barrett’s Esophagus, we take a closer look at what Barrett’s esophagus is, how it develops from chronic acid reflux, and why early detection is essential to reducing the risk of esophageal cancer. We’re joined by Dr. Raman Muthusamy, a nationally recognized expert in gastroenterology and advanced endoscopy, who explains how Barrett’s is diagnosed, the latest tools and technologies involved, and how a team-based approach improves outcomes. If you or someone you care about struggles with long-term heartburn or GERD, this episode offers critical insights to help you take action before it becomes something more serious. Missed Part 1? Scroll to the bottom of this page to listen or watch now. This series is sponsored by Castle Biosciences and produced in collaboration with leading clinicians and researchers dedicated to improving patient care and outcomes.
May 27, 2025
From Reflux to Risk: How Heartburn and GERD Could Lead to Esophageal Cancer
Is your heartburn more dangerous than you think? In this first episode of our 4-part patient-focused series, we break down the serious risks of untreated acid reflux and gastroesophageal reflux disease (GERD)—including its connection to Barrett’s esophagus, the only known precursor to esophageal cancer. Dr. Dan Lister, a leading Foregut Surgeon and founder of the Arkansas Heartburn Treatment Center, joins us to explain: – How GERD can progress silently over time – Why Barrett’s esophagus matters—and how it’s detected – What red flags to look out for (including when reflux suddenly disappears) – The latest treatment options that could help prevent cancer Whether you’ve been living with reflux for years or are newly diagnosed, this episode is packed with life-saving insights. This special 4-part series is sponsored by Castle Biosciences and produced in collaboration with leading clinicians and researchers dedicated to improving patient outcomes.
Listen to our
latest Podcast!